In This Section
- Home
- About us
- People
- Courses
- Current Students
- Research
- Shaping Society
- Careers
- News and Events
- International Applicants
- Alumni
- College of Business and Law
- Scholarships and Prizes
Dr Mary Tumelty's Research Highlights The Need To Revisit the Term "Second Victim" in Cases of Medical Error
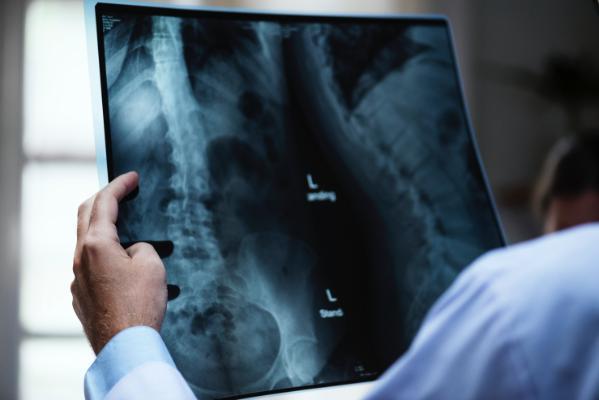
As a society, we can be guilty of perceiving medical practitioners to be infallible. In part, this may be a consequence of the esteem in which practitioners have traditionally been held, which reinforces our interpretation of what it means to be a medical professional.
Consequently, medical practitioners tend to possess a strong professional identity, which according to one doctor interviewed by Dr Mary Tumelty in her paper The Second Victim: A Contested Term, can come to define them.
"We’re by nature, perfectionists and very conscientious, and for a lot of us that’s our downfall… the identity of the doctor is very much rooted within themselves.
As part of the process of becoming a professional, we take on the role of a doctor in almost every cell in our body, even when we go on holidays we’re still doctor, when we register in the hotel or check-in, we become doctors 24 hours a day and if something happens…
that goes to our very soul and it’s very traumatic".
Living in such an identifiable role, where practitioners are almost expected to exhibit the characteristics, values and norms associated with a position that projects precision as a hallmark, creates an environment where mistakes are not tolerated.
Consequently, when a medical professional commits a serious medical error, quite often they are forced to internalise the effects of what could be a career-defining event for them and a life-changing moment for a patient.
Following such an error, medical professionals can struggle to deal with what has been described as a mild form of PTSD, where practitioners systematically relive the event in their minds and agonise over what they could have done to prevent the mistake from occurring.
"For doctors, generally speaking, making mistakes is very, very difficult… they find [it] very difficult to cope… The ones that remain with them are the traumatic ones, where they might have made a mistake".
Despite suffering from a variety of destructive emotions that can leave practitioners feeling isolated and bereft of confidence, with little support available, medical professions often continue to practice, which in some cases can put patients at risk.
Indeed, it wasn’t until Professor AW Wu coined the phrase ‘second victim syndrome’ in a landmark study published in 2000 that the profound and long-lasting impacts suffered by practitioners who committed medical error were completely recognised.
However, although the phrase has since been internationally accepted, given the connotations of the word “victim”, the term remains a source of debate.
Through a series of interviews with medical and legal professionals based in Ireland, Dr Mary Tumelty explored this debate by seeking out their perceptions of the term.
“I think it’s accepted that an adverse error or a medical mistake can have a significant impact on a medical practitioner, but what I found was that not all medical practitioners are comfortable using the term “second victim”.
Primarily, this stems from typical connotations of the word ‘victim’, which of course is a potent word laden with emotive and evaluative significance.
So, although the article talks about the difficulty with the term, it also recognises the significance of the phrase.
Consequently, while the article identifies a need to develop a new term, it suggests that medical professionals are the best-placed individuals to develop one”.
Given the often serious and life-long consequences a medical error can have on a patient, it is easy to understand why medical professionals are uncomfortable with describing themselves “victims”.
After all, adopting the word victim risks undermining patients who experienced physical and/or physiological harm as a result of medical error.
Additionally, as society traditionally associates victims as people who are “helpless” or “worthy of sympathy”, for a medical professional to adopt the term in the context of medical error where a patient suffered harm, could be interpreted as being disrespectful.
As one medical professional told Dr Tumelty during the course of her research, “the only thing I would feel about the term ‘second victim’ is that it would be perceived as ‘oh those doctors are just looking after themselves, and thinking of themselves’. I’m not mad about it”.
Nevertheless, as Dr Tumelty points out in her article, despite opposition to the term and the use of the word victim in particular, no other phrase has been suggested.
Indeed, since Professor Wu first coined the phrase, the term has become internationally recognised and it’s likely that its use will continue until such time as it is replaced.
As such, Dr Tumelty believes that as the term is “contested and in need of revisitation”, any replacement should come from the stakeholders involved, which include patients and physicians, as they are “best placed to assign meaning to this phenomenon”.
Read The Second Victim: A Contested Term in full.
School of Law
Scoil an Dlí
Contact us
Room 1.63, Aras na Laoi, T12 T656
